Every year, thousands of premature infants are at risk of losing their sight to retinopathy of prematurity (ROP). The good news: ROP is treatable. The persistent challenge is that the specialists needed to diagnose and treat it are in short supply, and training takes time, access, and repetition that traditional models of surgical training and education currently struggle to provide.
XR (extended reality) simulation and AI (artificial intelligence) are now beginning to change that equation.
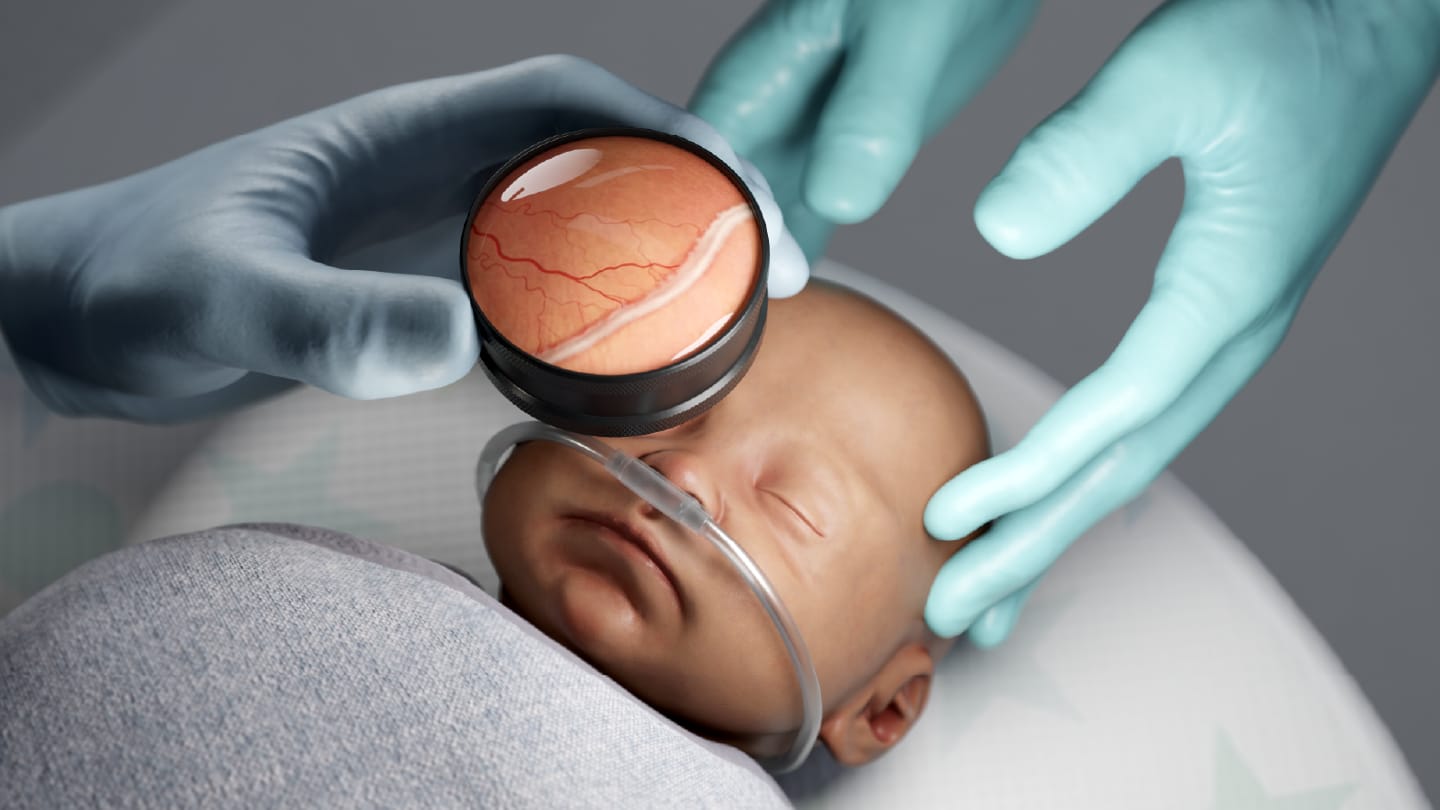
Small eyes, high stakes
Retina surgery is already among the most technically demanding disciplines in medicine. Surgeons operate at a microscopic scale within the posterior segment, navigating instruments through tissue so fragile that the margin for error can be measured in microns Ophthalmic surgical learning curves are steep, with performance only stabilizing after roughly 200 cases (1), and the skill required is as much instinct as it is technique.
ROP raises the stakes further as clinicians must adapt every technique to a much smaller anatomy, the eye of a premature infant – especially when these patients cannot communicate distress and can move unpredictably. Diagnosis requires indirect ophthalmoscopy, where the physician wears a head-mounted ophthalmoscope and manually aligns a condensing lens with the infant’s eye, maintaining that alignment across a systemic examination of multiple retinal quadrants. Treatment, when indicated, involves laser photocoagulation of the peripheral retina, relying on precise, sustained, targeting that can last 20 to 40 minutes, depending on disease severity.
These are not skills that are built quickly, and the case volume to build them organically simply isn’t available to most trainees.
Practice without consequence
This is where immersive simulation makes its strongest argument. The core promise of XR in surgical training is simple: repetition without any of the risk. Trainees can practice indirect ophthalmoscopy, lens positioning, optical alignment, and systemic retinal visualization as many times as they need, without placing an infant patient at risk.
Beyond procedural rehearsal, virtual patient libraries give trainees something clinical training rarely can: a reliable spectrum of pathology. From early vascular abnormalities to advanced retinal detachment, learners can encounter every stage of ROP disease progression on demand, without having to wait for the right case to come through the door.
Procedural simulation enhances this even further. Trainees can rehearse laser photocoagulation techniques, targeting accuracy, energy control, and treatment coverage without time pressure and without consequence. Early evidence suggests immersive training can accelerate surgical learning (2), reducing operating room training time and supporting faster progression towards procedural independence.
Moving beyond “keep practicing”
Simulation alone is valuable, yet when paired with intelligent assessment it can be transformative. AI-driven platforms are able to capture performance metrics that would be impossible to track in a clinical setting – metrics such as examination coverage, procedural timing, targeting accuracy, training frequency, and consistency across sessions. This data provides something traditional apprenticeship cannot – an objective, longitudinal record of how a trainee is developing at any given time.
The record supports structured competency assessment for program directors to reference, and enables targeted, specific feedback for trainees. There is a significant gap between generic feedback such as “keep practicing” versus more targeted feedback like “your peripheral coverage is inconsistent in the inferior quadrant.” Now, AI has made the latter possible at scale
Training at scale, anywhere
The urgency is not confined to training programs in wealthy academic medical centers. Advances in neonatal care across low- and middle-income countries have improved survival rates for premature infants. The number of ophthalmologists trained to screen and treat ROP has not kept up with demand, leading to a growing burden of preventable childhood blindness in regions least equipped to handle it (3).
Simulations offer scalable responses, and XR platforms can deliver standardized, high quality training without requiring proximity to a specialist teaching center. Web-based immersive simulation training extends the reach even further, enabling training in settings even without access to virtual reality (VR) hardware. In 2024, the American Academy of Ophthalmology recognized this potential, launching a VR education program with Fundamental XR that expanded access to ophthalmologic training globally.

More reps, better surgeons
It is worth noting that there are limitations with these technologies. XR simulation does not replace the clinical experience that defines ophthalmologic training, and no virtual environment can fully replace the judgement, tactile feedback, and situational complexity that you get from working with a real patient in a real setting. But it can simulate that scenario in significant ways.
Retinopathy of prematurity (ROP) is a major cause of preventable childhood blindness, and while effective treatment tools exist, training physicians has historically been a significant challenge. Recent advancements in technology – particularly virtual reality – are transforming this landscape by enabling ever more realistic simulations of a premature infant’s eye using a condensing lens. This innovation makes it possible to train specialists more efficiently in diagnosing and treating ROP. The current focus is on bridging the gap between this emerging technology and broader treatment access, with each simulation bringing the field closer to reducing avoidable childhood blindness and making a lasting impact.
This type of technology offers an extended and structured real-time simulated experience for the trainee. It fills gaps between observation and independent performance, as well as giving trainees the repetition they cannot get from the volume of cases alone, in an environment where mistakes made become learning opportunities rather than poor patient outcomes.
In this subspecialty alone, where the patients are vulnerable and unpredictable, safer training matters most. Technological advancements such as the use of extended reality, AI, and robotics are all crucial to enabling those coming into the world early to have a future where their sight is not limited by access to proper care.
References
- V Radeck et al., “The learning curve of retinal detachment surgery,” Graefes Arch Clin Exp Ophthalmol., 259, 2167 (2021). PMID: 33544177.
- RQ Mao et al., “Immersive virtual reality for surgical training: a systematic review,” J Surg Res., 268, 40 (2021). PMID: 34284320.
- AR Kemper et al., “Retinopathy of prematurity care: patterns of care and workforce analysis,” J AAPOS, 12, 344 (2008). PMID: 18440256.
